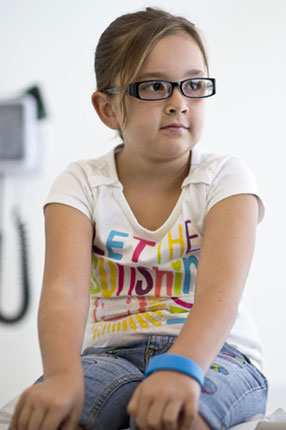It’s GREAT!
New clinical support for childhood cancer survivors
When Shannon and Gary Whisenant were absorbing news of their child’s grim prognosis, the potential side effects of her cancer treatment were not high on their what-if list of immediate concerns and overwhelming fears.
The couple’s 5-year-old daughter, Evan, was gravely ill. She would require an extremely tough treatment regimen involving numerous rounds of intensive chemotherapy followed by a bone marrow transplant. As part of the transplant, she would have total body radiation with extra doses to the brain, and additional intensive chemotherapy. Even if a good transplant match were found, the Whisenants were told, the odds of Evan surviving five years with hypodiploid acute lymphoblastic leukemia were just one in two.
“We said, ‘just fix her,’ ” says Shannon Whisenant, Evan’s mother. “And then we powered through it.”
Evan bravely survived the treatments. Now 10, she is in the fourth grade at Dudley Elementary School in Antelope. With her peace-sign decorated jeans, purple hair bow and painted pink fingernails, the thoughtful, inquisitive girl appears and behaves like any other her age. But five years after so many therapies and the transplant, Evan is not a normally developing child. Like many children who have endured cancer treatment, she copes with multiple late effects, including problems with her vision, diminished lung capacity, disrupted hormone production and other complications — many of which will be with her for the rest of her life.
Fortunately, the family has had ongoing support and care from the UC Davis Comprehensive Cancer Center’s “Getting Regular Evaluations After Treatment” clinic, or GREAT clinic, for short. While the cancer center has long monitored patients after treatment for signs of late effects, a $75,000 grant from Hyundai’s Hope on Wheels this year has enabled a more formal, coordinated clinical approach.
Kathryn Wells, a pediatric oncology nurse practitioner, is leading the effort. She sees GREAT patients on Friday mornings. Most are at least four years out from their cancer treatments. Wells explains that while not all pediatric cancer patients suffer late effects, many do because childhood malignancies are treated very aggressively.
“They need very intensive treatment to be cured, and they can tolerate the treatment, even more than many adults can,” she says. “And because we are treating them when they are going through growth and development, we need to assess what kind of damage that treatment may or may not have caused.”
The childhood cancer survival rate has surged to 80 percent over the past several decades, but more than 70 percent of the 350,000 survivors will develop adverse health effects, and 25 percent to 40 percent of those effects will be severe or life threatening, according to a 2006 study in the New England Journal of Medicine.
Evan has osteoporosis. She takes vitamin D and drinks milk to maintain and, hopefully, rebuild her bone density. Because of the radiation treatments she received, the 10-year-old has had three melanomas, skin cancers that must be caught and treated quickly. Radiation to her head caused cognitive delays, making reading more difficult. And treatment-related cataracts eventually will require eye surgery.
Radiation therapy and some chemotherapy agents also can cause infertility by directly damaging the ovaries or the testes. In addition to infertility, Evan likely will have difficulties reaching puberty and require hormone therapy.
Fortunately, some post-treatment problems have improved. Her liver has regained full function, and her kidneys are working well. While Evan’s limited lung capacity hampers her participation in school physical education, she loves to practice holding her breath while swimming in her backyard pool, and running around an expansive park near her Antelope home.
The long list of challenges would seem an overwhelming burden to most, but, as Shannon Whisenant says, “It’s who we are. It’s who she is. But we are blessed. She is here.”
And the family also feels relief knowing that Wells has logged everything in Evan’s “Passport for Care,” an Internet-based tool that facilitates the comprehensive follow-up medical care for child and young adult cancer survivors.
Marc Horowitz, professor of pediatrics at Texas Children’s Cancer Center, led development of the tool in collaboration with Baylor College of Medicine and the nationwide Children’s Oncology Group. He says Passport for Care addresses many problems confronting childhood cancer survivors including: the absence of good post-treatment care plans; the survivor’s limited understanding of their disease, treatment history and late effects risks; survivors’ frequent changes in medical providers, and the fact that most general practitioners are not trained to deal with late effects of cancer treatment.
Passport for Care works by assembling individualized survivor-care recommendations based on the survivor’s treatment history. It also provides end-of-treatment care summaries and customized educational resources. Horowitz says that 105 institutions now use Passport for Care, with more than 10,000 patients enrolled.
“I can input the therapy the patient has received and, based on the (treatment) exposures the patient has had, it lists the different sorts of health problems he or she may be at risk for,” says Wells. “It guides us in what kinds of questions we should ask, what sorts of physical findings we should look for, and which kinds of diagnostic tests we should consider.”
At her GREAT clinic visit recently, Wells carefully goes through Evan’s record, checking to ensure she received the follow-up care she needed from endocrinology, dermatology and ophthalmology, and that her blood and bone density tests are up to date. She talks with Evan and her mother about special education classes, her weight and diet, and tests Evan’s balance and listens to her heart. A social worker drops by to talk about a free camp for children with cancer diagnoses.
Wells hands Shannon Whisenant a printed summary of Evan’s treatment history and educational materials on each of the areas of concern. The thorough documentation and follow-up is a tremendous comfort.
“When you are going through it, the worst thing would be to feel abandoned — to not know everything,” Shannon Whisenant says. “The (cancer center and Kathryn Wells) guide me step-by-step through everything she needs. They make sure we are OK.”
Evan seems pleased with the attention, too. She presents Wells with three carefully sealed envelopes, each containing a hand-painted watercolor. Wells assures her young patient that she will proudly display each one of them on her office walls.