Emergency Medicine Residency Program
Choosing where to train for residency is one of the most important career decisions medical students will make. The clinical, social, educational, and professional experiences of residency training create the foundation for life-long learning and career sustainability after graduation.
The UC Davis Emergency Medicine residency training program is an allopathic, 3-year, university-based program whose vision is to educate emergency physicians who will provide compassionate, state-of-the-art emergency care, and advance the field of emergency medicine in their careers as clinicians, educators, and researchers. The program is fully accredited by the Accreditation Council for Graduate Medical Education (ACGME) and upon graduation residents are eligible for board certification by the American Board of Emergency Medicine (ABEM). Residents, fellows, and faculty are supported through a culture of wellness that promotes personal resiliency, professional fulfillment, and career sustainability.
The mission of the UC Davis Emergency Medicine residency program is to educate emergency physicians who will provide compassionate, state-of-the-art emergency care, and advance the field of emergency medicine in their careers as clinicians, educators, and researchers.
Graduates of the program will:
- Be prepared to practice in any clinical environment, including academic, community, and managed care settings;
- Have mastered advanced airway management skills necessary to control all airway scenarios;
- Be proficient in the pursuit of lifelong learning behaviors to ensure a sustainable and successful career;
- Develop communication skills and professionalism attributes necessary to navigate leadership roles successfully;
- Treat all patients and colleagues with respect, dignity, and compassion;
- Develop time and practice management strategies and resiliency in order to maximize personal well-being;
- Possess the necessary knowledge, skills, and behaviors to provide clinical care to patients of any age and from any background.
Integrated Air Force program graduates will be prepared for active duty deployment and ready to provide acute stabilization in combat theaters.
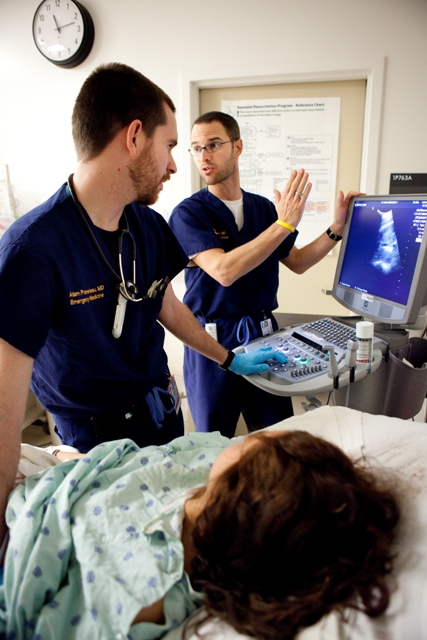 The clinical curriculum is designed to provide the educational experiences necessary to achieve clinical competence in the broad field of Emergency Medicine and includes dedicated clinical experiences such as medical ICU, surgical ICU, cardiac ICU, pediatric ICU, pediatric ED, anesthesia, ophthalmology, and toxicology, among others. Each rotation is selected for its educational value. With a multi-site program structure, we can choose the best location for each experience.
The clinical curriculum is designed to provide the educational experiences necessary to achieve clinical competence in the broad field of Emergency Medicine and includes dedicated clinical experiences such as medical ICU, surgical ICU, cardiac ICU, pediatric ICU, pediatric ED, anesthesia, ophthalmology, and toxicology, among others. Each rotation is selected for its educational value. With a multi-site program structure, we can choose the best location for each experience.
The high quality of off-service rotations is a strong aspect of the program. The curriculum is evaluated annually by residents and faculty and modified to maximize educational goals and objectives. Integral to the curriculum is a system of progressive responsibility for residents with supervision by board certified/board eligible Emergency Medicine attending physicians. Senior residents function independently by the end of their training.

At least five hours per week is scheduled for academic conferences. Academic Forum includes grand rounds, morbidity and mortality conference, simulation training, invited local and national speakers, quality improvement and patient safety conferences, oral board exam preparation, problem based learning, and presentations by residents. Clinical rotation schedules are arranged to allow maximum attendance at Academic Forum where faculty from all training sites present or facilitate small group discussions. Presenters utilize traditional lecture formats as well as interactive learning to teach the practice of Emergency Medicine. As such, the majority of content is presented or facilitated by emergency physicians.
Residents develop teaching and public speaking skills by presenting grand rounds, procedure conferences, morbidity and mortality conference case reports, and by facilitating case conferences. At monthly journal club, faculty and residents discuss selected topics in Emergency Medicine, develop skills to interpret the medical literature, and discuss practice implications of published findings. Advanced certifications in Advanced Cardiac Life Support (ACLS), Advance Trauma Life Support (ATLS), Pediatric Advanced Life Support (PALS), and Emergency Neurological Life Support (ENLS) are provided early in the training program. The Department of Emergency Medicine offers nationally recognized postgraduate Continuing Medical Education (CME) conferences at nearby resorts.
The UC Davis Department of Emergency Medicine is consistently ranked in the top five clinical departments nationally for federal National Institutes of Health (NIH) research funding in Emergency Medicine. Exposure to research methodology is integral to education during residency training, and residents learn on the job, during journal club, from research mentors, and during the development phase of their scholarly project. Clinical research continues to play a significant role in the academic development of the specialty. The resident scholarly project, presented in the senior year, may include a clinical research focus.
The Department provides statistical and computer support for clinical operations, its education programs and trainees, and its research mission. Clinical research is facilitated within the emergency department by opportunities for resident involvement in clinical research and quality improvement projects. Interprofessional quality improvement and patient safety conferences are held quarterly. Residents who wish to pursue a career in academic Emergency Medicine are encouraged, supported, and mentored to that goal. All residents are supported to be successful leaders regardless of their intended area of practice after graduation.
/Web_Teamsite/global health group.jpeg)
We define global health as the pursuit of improving and achieving equity and optimal health for all humans in their unique context and circumstance. We also recognize that healthcare professionals, industry leaders, educators, and researchers face many challenges as they attempt to improve the health of populations around the world. Improving global health requires special knowledge, a diverse skill set, and unique attitudes and perspectives beyond the traditional residency curriculum.
Our global health Area of Distinction and Certificate program is designed to prepare and inspire emergency medicine physicians-in-training for global health work during and after residency. Residents who complete the program will gain awareness of critical global health issues and acquire the tools necessary to incorporate global health into their careers. The longitudinal program combines both synchronous and asynchronous curricula, and global work at either an affiliated global site or one chosen by the trainee. Residents who complete the certificate in global health program will have demonstrated competency in the study, research, and practice of global health, with an emphasis on providing skills to address emerging global health challenges. The certificate program is a platform from which to perform a capstone experience with meaningful pre- and post-experience work.
For more information about the global health Area of Distinction and certificate program, contact: