Fetal Care and Treatment Center
Spina bifida
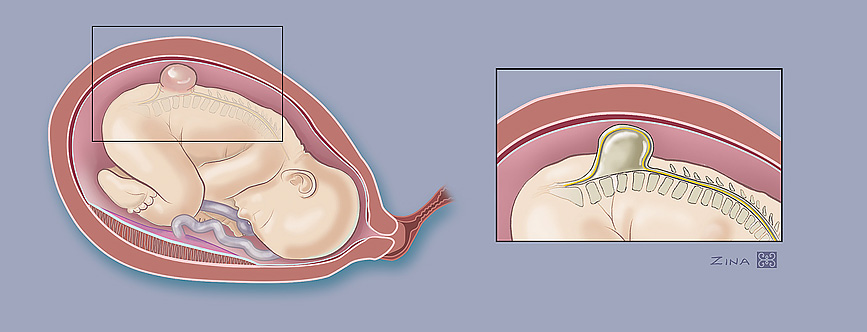
What is spina bifida, or myelomeningocele?
Spina bifida, also known as myelomeningocele or MMC, involves abnormal development of an unborn baby’s spine and spinal cord, the column of nerves that connect the body’s nerve system to the brain.
The spine consists of the spinal column, which is made up of bones separated by discs of fibrous tissue. Behind this column is the spinal canal, which contains the spinal cord that connects all the nerves in the body to the brain. The spinal canal is surrounded by arches of bone attached to the spinal column. In cases of spina bifida, these arches do not fully close.
There are two types of spina bifida:
- The visible sign of spina bifida cystica in a newborn child is a sac or cyst, rather like a large blister on the back, covered by a thin layer of skin. There are two forms of spina bifida cystica:
- In myelomeningocele, the spinal cord is damaged or doesn’t develop properly, causing nerve damage or paralysis.
- In meningocele, the characteristic cyst or membrane contains no nerves and can be removed by surgery, with little or no damage to nerve pathways.
- With spina bifida occulta, skin covers a tiny gap between the vertebrae, causing either no or very mild symptoms.
Diagnosis
In most cases, spina bifida is diagnosed before the baby is born. The primary screening is the maternal serum alpha-fetoprotein test, which analyzes blood for alpha fetoprotein, a protein that the fetus produces. Abnormally high levels of the protein may suggest that the fetus has spina bifida.
If the blood test shows high levels of alpha fetoprotein, an ultrasound examination is recommended. During this procedure, high-frequency sound waves bounce off tissues and create images that reveal signs of spina bifida.
Amniocentesis, in which a needle is introduced into the amniotic sac and a fluid sample removed for analysis, can detect a high alpha fetoprotein level and confirm the presence of spina bifida.
Treatment
For many decades, infants with myelomeningocele routinely had surgery shortly after birth, protecting the spinal cord by closing the normal tissues of the back.
Today, fetal surgery is an option for some cases of myelomeningocele. The procedure involves opening the mother's abdomen and uterus to allow access to the fetus. Surgeons can then close the neural tube and other layers of the fetus’ back. Although it cannot restore already lost neurological function, the procedure may prevent additional loss from occurring during the remainder of the pregnancy.
Outcomes
The level of cognitive and physical disability with spina bifida is associated with where the lesion occurs, its size, when treatment occurs and whether or not additional defects are present. A child born with hydrocephalus, in which spinal fluid collects in the brain, is likely to have some cognitive abnormalities. The higher the lesion on the spine, the greater the likelihood of mobility issues. The majority of children with spina bifida have bowel or bladder incontinence.
Fetal surgery for spina bifida was studied in the Management of Myelomeningocele Study, or MOMS. That research showed that surgery prior to birth reduced the need for ventriculo-peritoneal shunting, or a V-P shunt, and somewhat reduced the need for walking support later in life. In addition, it reduced the severity of changes in the shape of the head, called Arnold-Chiari malformation type II. Led by Diana Farmer, M.D., chair of the UC Davis Department of Surgery, MOMS is the reason why fetal surgery is offered for spina bifida.
Learn more about CuRe Trial
Visit clinical study pageContact us or make a referral
Physicians, patients and families can contact the Fetal Care and Treatment Center to find out more about our fetal care services.
Wondering about what types of conditions should be referred to us? View list of conditions to refer.
Referring physicians from other facilities, please use our Fetal Care and Treatment Center Referral form to refer patients and request services.
UC Davis Children’s Hospital
4301 X Street, 1st Floor, Suite 1501
Sacramento, CA 95817
The Fetal Care and Treatment Center is located within UC Davis Children’s Hospital.
View map and directions


