Before becoming a researcher, Ramsey Badawi saw firsthand the power of noninvasive nuclear imaging technology. Badawi got a job as a computer technician at a London hospital that introduced him to the power of positron emission tomography – or PET. It was the start of his new career in health care.
"I believe PET technology has the ability to make personalized medicine a reality," says Badawi, a UC Davis physicist and now 17-year PET veteran.
Unlike other forms of imaging, PET can accurately measure physiological functions such as blood flow, oxygen use and glucose metabolism. It can determine how well organs are functioning, help monitor the efficacy of drugs and distinguish benign from malignant tumors. In recent years, scientists have combined PET technology with X-ray CT, or computed tomography, allowing them to overlay PET scans onto computer-generated three-dimensional maps of the body's structure.
"PET gives you the physiological information, while CT gives you the anatomical information," Badawi says. "Together, the whole story they tell is truly greater than the information the two technologies can provide separately."
Bringing PET/CT to breast cancer
Currently, the combined technologies are only clinically available on full-body PET/CT scanners, which cannot easily pinpoint tumors smaller than one-half inch in size. As screening has improved and become more targeted, many women are diagnosed with small, early-stage breast tumors. Imaging these small tumors with PET/CT could improve staging and surgery planning, as well as allow physicians to evaluate the effectiveness of chemotherapy.
"We've known for years from full-body PET/CT that the two technologies complement each other, but full-body imagers just don't have the resolution you need to image primary breast cancer," Badawi says.
Badawi took up the challenge of developing the first clinical breast PET/CT scanner upon arriving at UC Davis in 2004 from the Dana Farber Cancer Institute at Harvard. He was lured to UC Davis by the prospect of working with Simon Cherry, who directs the UC Davis Center for Molecular and Genomic Imaging and built the first PET machine with enough resolution to accurately image tumors in mice.
"Deep in my heart, I wanted to build PET scanners, and UC Davis has one of the top PET engineers in the world in Simon Cherry," Badawi says.
Thanks to Cherry, Badawi found a new collaborator in UC Davis radiologist John Boone, who built the first dedicated breast CT scanner. At that point, the idea to create more than just another PET scanner was born.
"I took one look at Boone's dedicated breast CT scanner and knew there was plenty of room to mount a PET scanner. It seemed like the obvious thing to do," he says.
According to Cherry, the three-way collaboration of himself, Badawi and Boone is quickly making the transition of breast PET/CT from pre-clinical to clinical applications a reality.
"UC Davis has the right people at the right time to bring these technologies together," says Cherry, whose lab meets weekly with Badawi's. "Through these interactions, my group gets to see the clinical side, how their efforts are being used and how they can make a difference in the lives of breast cancer patients."
How dual imaging works
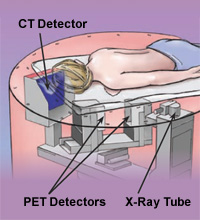
A breast PET/CT scan takes about 10 minutes per breast. Just the same as with breast CT, the patient lies on a padded table while the breast hangs down through a circular opening. In one study, Boone and UC Davis chief of breast imaging Karen Lindfors found that this type of system is more comfortable and preferred by patients to standard compression-based imaging systems.
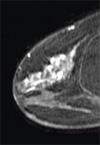
The CT images are generated first using an X-ray source and detector that are rotated around the breast to produce a three-dimensional map showing the internal structures of the breast.
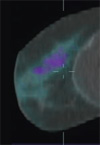
For PET images, the patient is first injected with a radiotracer – fluorodeoxy glucose, or FDG – which is absorbed into the body in proportion to the amount of sugar that the cells are using. Cancer cells use more sugar than normal cells, so the FDG reveals them as "hot spots" on PET scans. As with CT image production, a gamma ray detector rotates around the breast to produce a second three-dimensional map.
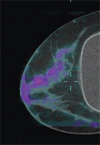
The combination of the two three-dimensional maps shows the precise location of cancer as "hot spots."
In December 2007, Badawi's lab produced the first-ever images of a patient's breast cancer using for the very first time a PET/CT scanner designed specifically for imaging the breast. Badawi admits that he spent a day-and-a-half staring in amazement over the first image his team produced.
"It was quite exciting. The resolution was startling," says Badawi. "You could see clearly the patient had several different manifestations of the disease. Compared to the whole-body scans, the detail was exquisite."
Badawi predicts that breast PET/CT will be most useful for surgery planning in women who have been diagnosed with breast cancer. The technology promises to improve neoadjuvant chemotherapy, which shrinks tumors prior to surgery. Physicians will be able to tell within a matter of weeks if the drugs are working.
Badawi also believes PET/CT may be useful in women who have had lumpectomies and whose scar tissue makes it difficult to look for recurrence using X-ray alone. It may also help in screening dense-breasted women who are at an increased risk of developing breast cancer due to inheritance of breast cancer genes.
Building on breakthroughs
It has been gratifying, Cherry says, to see what Badawi has done with the technology he first developed.
"We had PET technology we were using in small animals that gave us better spatial resolution than you find in clinical systems," he says. "Now we're applying that to breast cancer."
For his part, Badawi is looking forward to completing the first clinical trial using the current breast PET/CT machine. He is also, of course, anticipating building the next-generation machine and incorporating biopsy capabilities.
"We have now built PET detectors with twice the resolution of the existing system. We hope to start using them to build a new scanner in early 2009. We will be able to see a hot spot, take a sample, and know sooner rather than later if the patient has breast cancer," Badawi predicts. "The sooner the better."