Robotic-Assisted Gastrointestinal Surgery FAQs
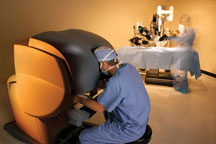 UC Davis Medical Center surgeons have been using robotic-assisted procedures since 2004. These minimally invasive, laparoscopic techniques have been used to treat a variety of conditions, ranging from prostate and ovarian cancers to conditions of the upper GI tract such as hiatal hernias and achalasia. The surgical robot is an operating- room machine completely controlled by a skilled surgeon who manipulates mechanical arms from a console near the patient’s bed. The procedure uses much smaller incisions than traditional “open” surgery, which helps reduce blood loss and postoperative recovery times. UC Davis surgeons perform dozens of robotic-assisted procedures each month using the state-of-the-art da Vinci® computer-enhanced surgery system.
UC Davis Medical Center surgeons have been using robotic-assisted procedures since 2004. These minimally invasive, laparoscopic techniques have been used to treat a variety of conditions, ranging from prostate and ovarian cancers to conditions of the upper GI tract such as hiatal hernias and achalasia. The surgical robot is an operating- room machine completely controlled by a skilled surgeon who manipulates mechanical arms from a console near the patient’s bed. The procedure uses much smaller incisions than traditional “open” surgery, which helps reduce blood loss and postoperative recovery times. UC Davis surgeons perform dozens of robotic-assisted procedures each month using the state-of-the-art da Vinci® computer-enhanced surgery system.
Working from a special console in the operating room, a surgeon operates several precision-guided robotic arms 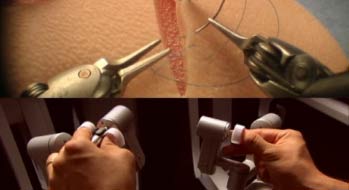 that hold and manipulate miniaturized instruments that are inserted through keyhole-sized incisions in the patient. A small video camera, inserted through another tiny incision, provides surgeons with a magnified 3-D image of the operating site. This expansive view allows doctors to see and avoid surrounding nerves and muscles. The robotic arms, with their ability to rotate 360-degrees, enable surgical instruments to be moved with greater precision, flexibility and range of motion than done in standard minimally invasive laparoscopy.
that hold and manipulate miniaturized instruments that are inserted through keyhole-sized incisions in the patient. A small video camera, inserted through another tiny incision, provides surgeons with a magnified 3-D image of the operating site. This expansive view allows doctors to see and avoid surrounding nerves and muscles. The robotic arms, with their ability to rotate 360-degrees, enable surgical instruments to be moved with greater precision, flexibility and range of motion than done in standard minimally invasive laparoscopy.
Most procedures take two to three hours under general anesthesia. Patients typically experience only minimal blood loss, and blood transfusions are rarely needed. Depending on the condition being treated, patients often only spend one night in the hospital and are usually discharged as soon as their laboratory tests are acceptable, pain is controlled, and they are able to retain liquids.
Patients typically experience significantly less pain and blood loss than in conventional “open incision” procedures. Patients also tend to enjoy quicker recovery times. Traditional, open surgery requires several days of hospitalization, and a recovery time that can last several months. While every case is unique, with robotic-assisted surgery, the return to normal everyday activities (except for lifting heavy objects and strenuous exercise) can occur in as little as two to three weeks.
The use of the robotic equipment in surgery means a more precise and less disruptive dissection, which helps control potential sources of bleeding.
As with any major surgery performed under general anesthesia, there is a certain amount of risk, including heart attack, stroke, and death. Preoperative assessment of a patient’s overall health is part of the standard surgical evaluation at UC Davis.
The decision to surgically treat a patient involves many considerations. Not every patient is an appropriate candidate for a minimally invasive procedure. UC Davis surgeons work closely with every patient, discussing treatment options and helping them decide on the best course of action, which may include robotic-assisted surgery.

