Residency Program - Case of the Month
May 2012 - Presented by Michael Van Nes, M.D.
Answer:
Solitary fibrous tumor
Histo-pathologic findings:
Microscopic examination revealed a heterogeneous tumor consisting mostly of of interlacing bundles of spindle cells with hyperchromatic, regular nuclei. Mitotic figures were very sparse throughout the tumor. A background of fine capillary network was present. The spindle tumor cells stained diffusely positive for CD34 (not shown) and CD99 (not shown) by immunohistochemistry. The case was signed out as solitary fibrous tumor.
Discussion:
Solitary fibrous tumor (SFT), is an uncommon tumor first described as pleural based, but now has been identified in numerous extrapleural sites, including pulmonary parenchyma, peritoneum, kidney, liver, bone, nasopharynx, orbit, urogenital system, breast, mediastinum, skin, meninges, and spinal cord.1-3 Alternate older names included: localized fibrous tumor and localized fibrous mesothelioma.
Regardless of site, SFT grossly presents as a tan, white, and rubbery to slightly firm nodule with a smooth, unencapsulated surface. Histologically, SFTs are well circumscribed and consist of bland spindle cells with variable hypo- and hyper-cellular, myxoid, or hyalinized areas. Foci with so called hemangiopericytomatous vascular pattern and dense collagen are often. Mitoses are rare and necrosis is unusual in SFT.
Immunohistochemical (IHC) staining shows strong diffuse cytoplasmic positivity for CD34 and vimentin in almost all cases and variable positivity for Bcl2.3 Epithelial membrane antigen is typically negative but has rarely been reported as positive. No immunoreactivity is seen for cytokeratin, CD31, S100 protein, factor VIII, desmin, or smooth muscle actin.
The histologic differential diagnosis of SFT is broad and includes: fibrous histiocytoma, hemangiopericytoma, schwannoma, GI stromal tumor (GIST), and leiomyoma. These can be ruled out by histology and IHC.
Benign fibrous histiocytoma usually has a characteristic storiform pattern of fibroblasts, occasionally admixed with round histiocytic cells and multinucleated giant cells, and is usually negative for CD34 or only focally positive for CD34.
Hemangiopericytoma is controversial lesion, classically composed of monotonous round to spindle cells around thin-walled, endothelium-lined vascular channels that usually have a staghorn pattern. Foci of hemangiopericytomatous differentiation can a seen in some SFTs; however, SFT characteristically exhibits more diffuse and strong positivity for CD34 than does hemangiopericytoma.4
Hemangiopericytoma (HPC), first described as a neoplasm with distinct morphologic features, presumably composed of pericytes, is now being considered a pattern rather than a diagnosis.5 In soft tissue, it is generally accepted that most such lesions are solitary fibrous tumors (SFTs), monophasic synovial sarcomas (SSs), or myofibromatoses. Similarly, to their soft-tissue counterpart, HPCs in bone have been reclassified as either SFT or SS of bone.5 Some have embraced a histologic separation of hemangiopericytoma and SFT, viewing them as ends of a continuum, rather than 2 lesions with distinctly defined histopathology.6
Although some cases of schwannoma are CD34 positive, the characteristic morphology of alternating Antoni A and Antoni B areas, Verocay bodies, and diffuse S100 positivity make the diagnostic distinction simple. Diffuse and intense reactivity for muscle markers such as muscle-specific actin helps differentiate leiomyoma from SFT.
Overtly malignant SFTs, including some with distant metastases, have been reported in 20% of pleural cases with high (50%) mortality rates.3, 7 Malignant forms of SFT are characterized by higher cellularity, nuclear atypia, mitotic activity, and necrosis.2 Extrapleural cases seem less likely to run an aggressive course, but malignant SFTs in extrapleural sites including the orbit have been documented.8 The treatment of choice of SFT is complete surgical excision with follow-up.
References:
http://surgpathcriteria.stanford.edu/softfib/solitary_fibrous_tumor/
- Brunnemann RB, Ro JY, Ordonez NG, Mooney J, El-Naggar AK, Ayala AG. Extrapleural solitary fibrous tumor: a clinicopathologic study of 24 cases. Mod Pathol. Nov 1999;12(11):1034-1042.
- Hanau CA, Miettinen M. Solitary fibrous tumor: histological and immunohistochemical spectrum of benign and malignant variants presenting at different sites. Hum Pathol. Apr 1995;26(4):440-449.
- Warraich I, Dunn DM, Oliver JW. Solitary fibrous tumor of the orbit with epithelioid features. Arch Pathol Lab Med. Jul 2006;130(7):1039-1041.
- Marchevsky AM, Varshney D, Fuller C. Mediastinal epithelioid solitary fibrous tumor. Arch Pathol Lab Med. Apr 2003;127(4):e212-215.
- Verbeke SL, Fletcher CD, Alberghini M, et al. A reappraisal of hemangiopericytoma of bone; analysis of cases reclassified as synovial sarcoma and solitary fibrous tumor of bone. Am J Surg Pathol. Jun 2010;34(6):777-783.
- Goldsmith JD, van de Rijn M, Syed N. Orbital hemangiopericytoma and solitary fibrous tumor: a morphologic continuum. Int J Surg Pathol. Oct 2001;9(4):295-302.
- O'Donovan DA, Bilbao JM, Fazl M, Antonyshyn OM. Solitary fibrous tumor of the orbit. J Craniofac Surg. Sep 2002;13(5):641-644.
- Ogawa K, Tada T, Takahashi S, et al. Malignant solitary fibrous tumor of the meninges. Virchows Arch. May 2004;444(5):459-464.

 Meet our Residency Program Director
Meet our Residency Program Director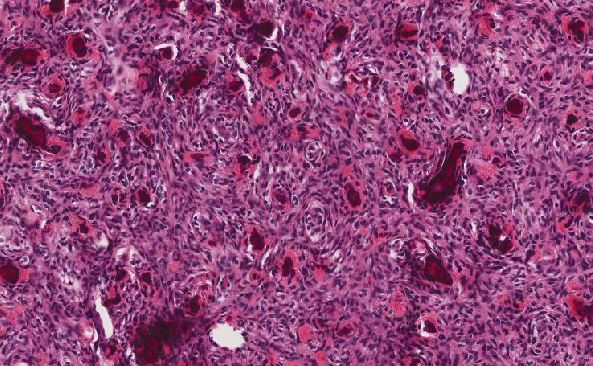
 LeShelle May
LeShelle May Chancellor Gary May
Chancellor Gary May