Residency Program - Case of the Month
July 2011 - Presented by Aram Millstein, M.D.
Answer:
Mixed carcinoid and goblet cell tumor arising in a mature teratoma
Histological description
The tumor is composed of monomorphic epithelioid-appearing cells that are forming nests, glands, and trabeculae. The nuclei contain dispersed chromatin and salt and pepper distribution suggesting neuroendocrine differentiation. There are some areas of individual tumor cells that infiltrate the ovarian stroma. These individual cells have a signet ring appearance and appear to have mucin in their cytoplasm. The cystic lesion appears to have had its lining denuded. There are eccrine and apocrine glands, adipose tissue and cartilage haphazardly arranged in the tissue surrounding the cyst.
Discussion:
Much of the tumor has the classic appearance of a carcinoid tumor, however the individual cells that are clearly infiltrating through the ovarian stroma and stain with neuroendocrine markers appear to contain mucin. Some of these individual cells have a signet ring appearance; therefore, the tumor is best classified as a mixed carcinoid and goblet cell tumor. Since there is a mature teratoma present in the ovary, the tumor most likely arose in this teratoma.
Primary mucinous (goblet cell) carcinoid of the ovary is a rare tumor. There are three much more common forms of primary carcinoid tumors of the ovary, insular carcinoids, trabecular carcinoids, and strumal carcinoids. Insular carcinoids consist of islands of neoplastic cells often separated by abundant fibrous stroma. These tumors are often associated with carcinoid syndrome (1). Trabecular carcinoids are characterized by ribbons of tumor cells. These tumors are not usually associated with carcinoid syndrome. Thirdly, strumal carcinoids are composed of neoplastic thyroid tissue and carcinoid that is in an insular or trabecular pattern. Less than 5% of these types of carcinoids are malignant (1). Primary mucinous carcinoid of the ovary is a much less common fourth subtype. In a report of 17 cases of primary mucinoid carcinoids, Scully et al identified three subgroups based on their morphology (1). Although the study contained a small sample size, the subgroups did correlate with prognosis.
Metastatic mucinous carcinoid tumors from the appendix are more common. It is important to distinguish a primary mucinous carcinoid of the ovary from a metastasis. Approximately 24 cases of appendiceal mucinous carcinoid metastatic to the ovary have been reported in the literature (1). Eighty percent of the tumors were bilateral. In differentiating metastatic mucinous carcinoid tumors to the ovary from primary ones, the criteria used for differentiating metastatic tumors in general from primary ovarian tumors should be used. Bilateral ovarian tumors, multiple ovarian nodules, vascular invasion within the ovary, and the finding of a primary tumor of the gastrointestinal tract favor metastatic mucinous carcinoid tumor. The finding of mucinous carcinoid tumor in a background of an ovarian neoplasm such as mature teratoma or an ovarian surface epithelial tumor establishes that the mucinous carcinoid tumor is primary to the ovary (1).
References:
- P Baker, E Oliva, F Young, A Talerman, and R Scully. Ovarian Mucinous Carcinoids Including Some With a Carcinomatous Component, A Report of 17 Cases. Am J Surg Pathol 2001;25(5): 557-568.

 Meet our Residency Program Director
Meet our Residency Program Director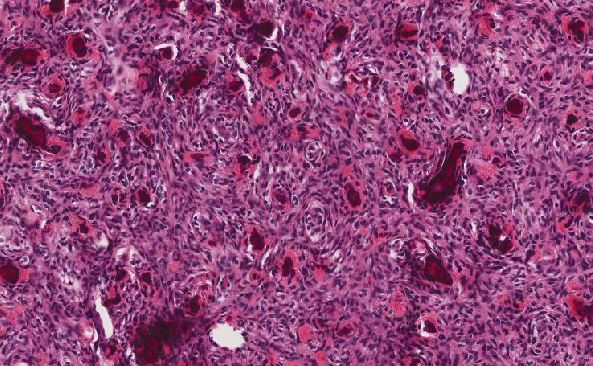
 LeShelle May
LeShelle May Chancellor Gary May
Chancellor Gary May