About Stem Cell Transplantation
Hematopoietic stem cells are immature cells that develop into:
- red blood cells – also called erythrocytes, which carry oxygen to organs and tissues
- white blood cells – also called leukocytes, which fight infections
- platelets, which help the blood to clot
All these cells play a crucial role in the healthy functioning of our bodies. Most stem cells are found in bone marrow, which is the spongy tissue inside large bones. Some cells also are found in the blood stream. Blood from the umbilical cord also contains hematopoietic stem cells. Cells from any of these sources can be used in transplants.
Stem cell transplantation is a treatment for a wide range of diseases including blood cancers such as leukemia, lymphoma and myeloma. It can cure some diseases and put others into remission.
Depending on the stem cell source, the procedure may be called a bone marrow transplant, a peripheral blood stem cell transplant, or a cord blood transplant.
In stem cell transplantation, patients are given intensive doses of chemotherapy and/or radiation therapy to kill cancer cells. At the same time, this treatment destroys the normal cells in bone marrow. To re-establish production of cells in bone marrow, patients must receive an infusion of healthy stem cells previously collected from a patient or stem cell donor.
There are three transplant types, which differ depending on the stem cell donor source. Each type involves a different procedure and carries different side effects and risks. The type of transplant recommended depends on a number of factors, including the patient’s type of disease, age and overall health, and donor availability.
Autologous transplant
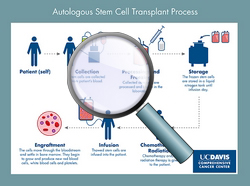 “Auto” means self. The patient donates his/her own stem cells prior to a high dose of chemotherapy or radiation.
“Auto” means self. The patient donates his/her own stem cells prior to a high dose of chemotherapy or radiation.
CLICK HERE TO ENLARGE ILLUSTRATION
Allogeneic: related donor transplant
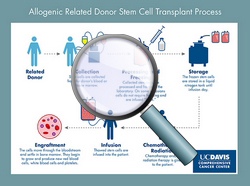 “Allo” means “other”. Stem cells are donated by another person, the donor. This donor is a genetically matched family member (usually a brother or a sister).
“Allo” means “other”. Stem cells are donated by another person, the donor. This donor is a genetically matched family member (usually a brother or a sister).
CLICK HERE TO ENLARGE ILLUSTRATION
Allogeneic: unrelated-donor transplant
 The person donating stem cells is not biologically related to the patient but genetically partially matches the patient. Unrelated donors may be found through the National Marrow Donor Program.
The person donating stem cells is not biologically related to the patient but genetically partially matches the patient. Unrelated donors may be found through the National Marrow Donor Program.
Before the transplant, chemotherapy, radiation or both are given. This pre-transplant treatment may be done in two ways:
Myeloablative (ablative, high intensity):
Myeloablative means marrow-destroying. During this treatment, a high dose of chemotherapy, radiation or both are given to destroy any cancer cells. This treatment also kills all remaining healthy marrow. Patients receive an infusion of new stem cells to rebuild the blood and immune system. In cases in which a patient's own stem cells are healthy enough, they are transplanted (autologous transplant); otherwise, transplanted cells come from a donor (allogenic transplant).
Non-myeloablative (reduced-intensity):
During the non–myeloablative treatment patients receive lower doses of chemotherapy and radiation, followed by an infusion of stem cells from a matched donor. This treatment eliminates some, but not all, of the patient’s bone marrow. It also reduces the number of cancer cells and suppresses the patient’s immune system to prevent the rejection of the transplanted cells. The reduced-intensity treatment allows older patients and patients with other health problems to have a transplant.
Stem cells used for transplants can come from three sources:
Peripheral (circulating) blood
Stem cells are collected from peripheral blood in a process called apheresis. The stem-cell donor blood circulates through a machine called a cell separator that removes the peripheral blood stem cells and returns the rest of the blood to the body. Because the concentration of stem cells in circulating blood is ordinarily very low, donors are given medications to stimulate the bone marrow to produce more stem cells. These cells are then released into the blood stream. The collection of stem cells from circulating blood is an outpatient procedure, and the donor (or patient) usually goes home the same day.
Peripheral stem cells are used most often in stem-cell transplantation for both autologous and allogeneic transplants.
Bone marrow
Bone marrow collection (also known as bone marrow harvest) is a surgical procedure that takes place in a hospital operating room. The collection is performed under general or spinal anesthesia. The stem cell donor does not feel significant pain or discomfort during the marrow collection. The bone marrow is removed with large needles from the flat pelvic bones. The donor may go home the same day or stay overnight in the hospital. Historically, this was how all stem cells were collected for transplantation, hence the common use of the term “bone marrow transplantation.”
Blood in the umbilical cord collected after birth
A newborn’s parents can donate umbilical cord blood to a public cord blood bank (where available) at no cost. Umbilical cord blood is rich in stem cells, and increasingly hospitals have the ability to collect these stem cells using special kits. The collection process does not pose any health risk to the infant and uses blood that would otherwise be thrown away. After the baby is born and the umbilical cord has been cut, blood is retrieved from the umbilical cord and placenta. The cord blood is then processed, frozen and stored until needed for a transplant patient.
Because cord blood cells are less immunologically mature than cells collected from adult donors, they can be used for transplantation even when the match between patient and donor is not perfect.